Written by: Christiane Grünloh
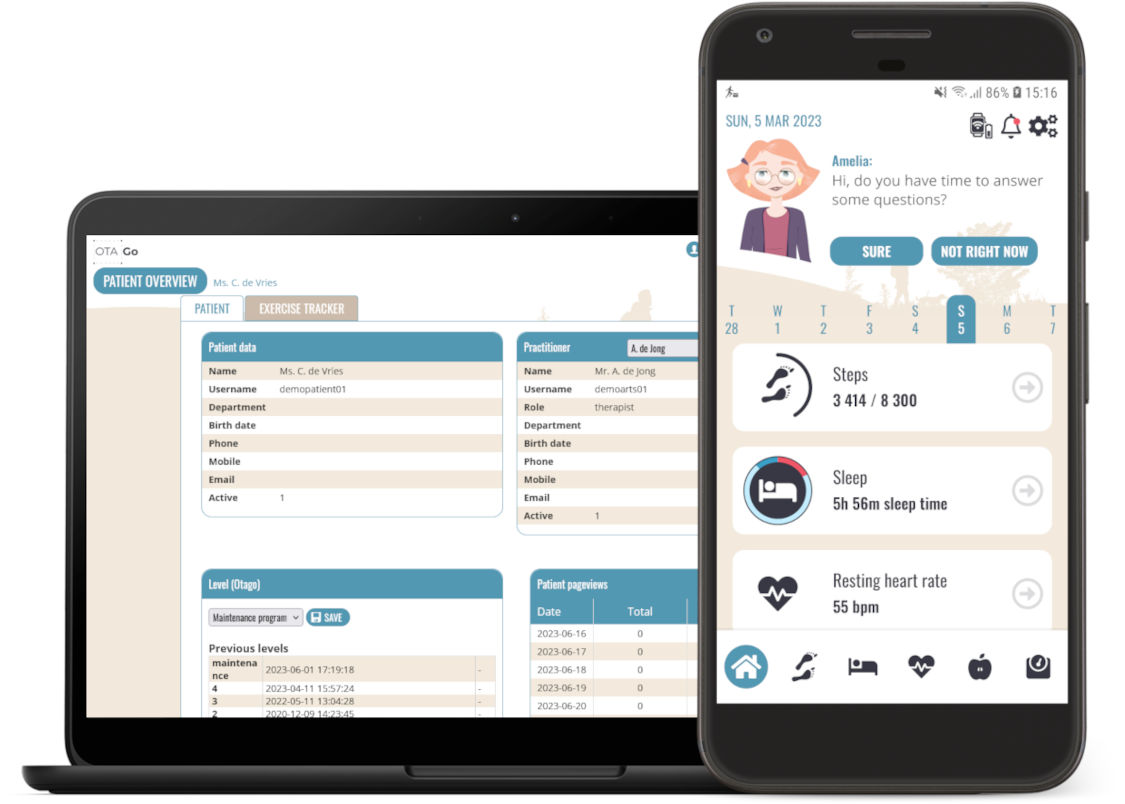
In the last week of June, Kira Oberschmidt and Christiane Grünloh attended the Final Conference of Pharaon in Florence. Pharaon is a large scale pilot project funded by European Union’s Horizon 2020 research and innovation programme under the grant agreement No 857188. The project started in December 2019 and with a one year extension ends in November 2024. We were excited to have the final conference of Pharaon in combination with ForItAAL, the Forum of Italian Ambient Assisted Living and the program was packed.
The Final Conference provided the opportunity to:
- learn more about the Pharaon pilot results and lessons learnt, the impact of the project, experiences from other large-scale pilots,
- connect with the different stakeholders
- start discussion and exploitation of the project’s services.
We presented the results of the 6 pilots in 5 countries (Spain (Murcia and Andalusia), Italy, The Netherlands, Slovenia, Portugal) in the session Innovation in Action: Pharaon pilot results. Given that Christiane is the general pilot coordinator in this project, she was the session chair and guided the audience through the presentations and Q&A at the end. Christiane was also invited to join the panel of experts on Innovation Europe: achievements from large scale pilots. Here she presented lessons learned and policy recommendations from conducting action research in the Pharaon pilots (see PDF (available in English only)).
Finally, we had 4 accepted papers accepted to ForItAAL which were presented by Kira and Christiane:
- Stakeholder Skill Training in Participatory Health Research: Themes and Topics for Future Research., by Kira Oberschmidt, Christiane Grünloh, Kevin Doherty, Ria Wolkorte, Sheree, May Saßmannshausen, Lara Siering, Åsa Cajander, Michal Dolezel, Svante Lifvergren, Karin van den Driesche
- "I thought: everybody wants to participate, right?" - Exploring patient motivation for taking part in long-term qualitative research, by Kira Oberschmidt, Christiane Grünloh, Marijke Broekhuis, Michael Bui, Monique Tabak
- They are the champions - identifying and supporting champions in eHealth Action Research projects, by Kira Oberschmidt, Christiane Grünloh, Mateja Erce, Francisco José Melero Muñoz, Elisabete Raquel Simão Pitarma, Monique Tabak
- Novice action researchers' theoretical understanding and practical implementation of action research in eHealth, by Kira Oberschmidt, Christiane Grünloh, Lex van Velsen
The last paper was even nominated as "ForItAAL Best Student Paper Award"!
We had very interesting discussions during the Pharaon final conference and ForItAAL. Do you want more information about this project or about these papers? Contact Christiane Grünloh!